Glucostatic theory of appetite control: Difference between revisions
imported>Gareth Leng |
imported>Gareth Leng No edit summary |
||
| Line 1: | Line 1: | ||
{{subpages}} | {{subpages}} | ||
In the early | In the early 20th century, a link was made between blood glucose and [[appetite]] that led to the '''glucostatic theory of appetite control'''. In 1916, Carlson suggested that plasma concentrations of glucose could serve as a signal for both meal initiation (low levels) and meal termination (high levels) <ref name="pmid15924903">{{cite journal|author=Mobbs CV ''et al.''|title=Impaired glucose signaling as a cause of obesity and the metabolic syndrome: the glucoadipostatic hypothesis |journal=Physiol Behav |year= 2005 |volume= 85 |pages= 3-23 | pmid=15924903 |url=http://www.ncbi.nlm.nih.gov/entrez/eutils/elink.fcgi?dbfrom=pubmed&tool=sumsearch.org/cite&retmode=ref&cmd=prlinks&id=15924903 | doi=10.1016/j.physbeh.2005.04.005 }}</ref>. However, it was not until the 1950's that Mayer put forward the ''glucostatic theory''. This theory proposed that a rise in plasma glucose concentration, for example after a meal, was sensed by "glucoreceptor" neurons in the [[hypothalamus]], which then signalled for meal termination. Glucose was thus thought of as a likely [[satiety]] factor <ref name="pmid17158418">{{cite journal| author=Flint A''et al.''| title=Glycemic and insulinemic responses as determinants of appetite in humans|journal=Am J Clin Nutr |year= 2006 |volume= 84|pages= 1365-73 |pmid=17158418 | url=http://www.ncbi.nlm.nih.gov/entrez/eutils/elink.fcgi?dbfrom=pubmed&tool=sumsearch.org/cite&retmode=ref&cmd=prlinks&id=17158418}} </ref>. The theory, popular in the 1950s, was losing support by the 1980s, when scientists were beginning to think that the control of appetite was a complex mechanism that would have to depend on the integration of many signalling pathways. The glucostatic theory was not abandoned altogether, as it was still thought to be important for short-term appetite control, but newly discovered peptides such as [[leptin]] became more likely candidates for long-term control. | ||
The theory, popular in the 1950s, was losing support by the 1980s, when scientists were beginning to think that the control of appetite was a complex mechanism that would have to depend on the integration of many signalling pathways. The glucostatic theory was not abandoned altogether, as it was still thought to be important for short-term appetite control, but newly discovered peptides such as [[leptin]] became more likely candidates for long-term control. | |||
==Physiological background== | ==Physiological background== | ||
Revision as of 10:52, 19 August 2012
In the early 20th century, a link was made between blood glucose and appetite that led to the glucostatic theory of appetite control. In 1916, Carlson suggested that plasma concentrations of glucose could serve as a signal for both meal initiation (low levels) and meal termination (high levels) [1]. However, it was not until the 1950's that Mayer put forward the glucostatic theory. This theory proposed that a rise in plasma glucose concentration, for example after a meal, was sensed by "glucoreceptor" neurons in the hypothalamus, which then signalled for meal termination. Glucose was thus thought of as a likely satiety factor [2]. The theory, popular in the 1950s, was losing support by the 1980s, when scientists were beginning to think that the control of appetite was a complex mechanism that would have to depend on the integration of many signalling pathways. The glucostatic theory was not abandoned altogether, as it was still thought to be important for short-term appetite control, but newly discovered peptides such as leptin became more likely candidates for long-term control.
Physiological background
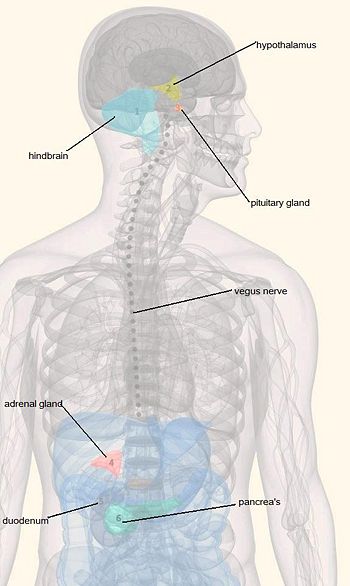
Glucose homeostasis must be finely regulated by the absorption of food and the flow of recently stored energy substances through different metabolic pathways. For the brain, glucose has to be supplied continuously from the blood since there is no storage for sugar available in the brain. Changes in glucose level elicit complex neuroendocrine responses that restore blood glucose levels to the optimum range [3]. The hypothalamus and the caudal brainstem both contain important centres which are responsible for monitoring blood glucose and regulating appetite [4]. Ritter et al. claimed that some glucoreceptor cells are located in the hindbrain. This means that the glucose sensing cells have direct access to the central nervous system and could elicit immediate responses to retain the physiological norm[5]. Catecholamine neurons in the hindbrain may help mediate responses to glucose deficiency by linking glucoreceptor cells to forebrain and spinal neurons. This enables us to stimulate behavioural and hormonal responses that elevate blood sugar level. These include increased food intake, adrenal medullary secretion, corticosterone secretion and suppression of estrous cycles. Complex behaviours involved in detection and identification of food are mainly regulated by the forebrain. The hindbrain may mediate the motivation for these activities via the neuronal circuit activated by some of the glucose sensing cells. This motivation circuit would have engaged the physical sign of energy deficiency with these behaviours [6].
Short-term control of appetite and satiety
The Glycaemic Index (GI) is a measure of the effects of glycaemic carbohydrates on postprandial blood glucose levels. Foods that are digested rapidly to produce a sharp rise in blood glucose are classified as high-GI, whereas foods that are digested and absorbed slowly have a low-GI.
Recent studies suggest that low GI diets prolong satiety and thereby reduce food intake; in one study, children given low-GI breakfasts ate less lunch and showed less hunger than children who had high-GI breakfasts. [7] In obese adolescents, low-GI meals are associated with a lower insulin response than high-GI meals, and the time intervals between meals were longer in low-GI test meal group, indicating that low-GI meals increased satiety. [8] Another study investigated the effect of variations in postprandial glycaemia and insulinaemia on subjective appetitive sensations in overweight and obese women. They modulated the rate of ingestion of a glucose beverage to examine the postprandial effects of high and low-GI meals. Sharp peaks followed by rapid decrease in glucose and insulin levels to below baseline were observed in subjects with rapid consumption while relatively stable glucose and insulin levels were seen in subjects with slow consumption. Higher hunger ratings and prospective intake were reported by the subjects with rapid consumption than those with slow consumption after meals demonstrating the positive relationship between blood glucose concentrations and satiety [9].
On the other hand, Flint et al. argue that after ingestion of various GI meals by healthy young male participants showed no association between glycaemic response and postprandial fullness though it may reduce energy intake in a subsequent meal. In contrast, insulinaemic response after the meal were positively correlated with postprandial satiety [2].
Thus, these short-term studies suggest that glycaemic and insulinaemic responses are implicated in appetite and satiety. The relatively early decline of blood glucose level to below the baseline after high-GI meal seems to play a role in initiating hunger and appetite.
Long-Term Control of Feeding and Energy Balance
The glucostatic hypothesis represents a physiological control system that fits the criteria for controlling short-term energy consumption. Few studies have looked at the glucostatic theory and the effect of varying GI foods in the long-term, but Alfenas and Mattes looked at the long-term effects on appetite of consuming high- or low-GI foods over days and weeks. Their findings suggested there were no significant differences in either glycaemic and insulinemic responses, or in hunger, fullness, and desire to eat [10].
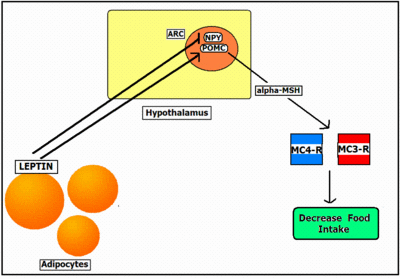
The long-term control of feeding appears to involve the secretion of leptin from fat (adipose) tissue. The concentration of leptin in the circulation is proportional to the amount of fat in the body. Leptin crosses the blood-brain-barrier via a receptor-mediated transport system [11], and leptin receptors are densely expressed in the hypothalamus and in the caudal brainstem; these are both areas that are known to control feeding and energy balance. The binding of leptin to these receptors influences the neuropeptide systems, pro-opiomelanocortin (POMC) and neuropeptide Y (NPY), a potent feeding stimulant. POMC neurons in the arcuate nucleus produce the peptide alpha-MSH, an appetite suppressant. An increase in leptin levels is thought to inhibit the release of orexigenic peptides, such as NYP, and increase the release of anorexigenic neuropeptides such as alpha-MSH [12].
The role of insulin and ghrelin in the glucostatic theory
Both ghrelin and insulin play important roles in appetite regulation.
Insulin is required by cells in order to take up and use glucose from the blood, and circulating levels of insulin are correlated with satiety and food intake. In the short-term, insulin is involved in limiting postprandial appetite [2]. However, glycaemic responses appear to be more important for this. Another study found that in obese and overweight women serum insulin levels were negatively correlated with subjects hunger ratings. They were also positively correlated to fullness. Again glucose had a bigger part to play in this than insulin. Both these studies suggest that, although other factors appear to be important, insulin may play a role in appetite control. However, other studies have found no relationship between insulin and appetite. Because of this, it is unclear how important insulin is in the control of appetite.
Ghrelin, a peptide produced in the stomach, stimulates appetite, and citculating ghrelin levels peak before a meal or when a meal is expected. In rats, insulin-induced hypoglycaemia up-regulates ghrelin mRNA expression. Ghrelin secretion is also inhibited by high glucose levels. This suggests that the cells which secrete ghrelin may be sensitive to changes in plasma glucose, and this may play an important role in regulating energy metabolism.
When ghrelin is deleted, blood glucose is reduced and insulin levels are increased. However, a study by Sun et al. found that these effects were not related to changes in food intake or weight. As with insulin, there is little conclusive evidence suggesting an important role for ghrelin in the glucostatic hypothesis.
References
- ↑ Mobbs CV et al. (2005). "Impaired glucose signaling as a cause of obesity and the metabolic syndrome: the glucoadipostatic hypothesis". Physiol Behav 85: 3-23. DOI:10.1016/j.physbeh.2005.04.005. PMID 15924903. Research Blogging.
- ↑ 2.0 2.1 2.2 Flint Aet al. (2006). "Glycemic and insulinemic responses as determinants of appetite in humans". Am J Clin Nutr 84: 1365-73. PMID 17158418.
Cite error: Invalid
<ref>tag; name "pmid17158418" defined multiple times with different content Cite error: Invalid<ref>tag; name "pmid17158418" defined multiple times with different content - ↑ Ritter S et al. (2006). "Hindbrain catecholamine neurons control multiple glucoregulatory responses.". Physiol Behav 89: 490-500. DOI:10.1016/j.physbeh.2006.05.036. PMID 16887153. Research Blogging.
- ↑ Mayer J (1955). "Regulation of energy intake and the body weight: the glucostatic theory and the lipostatic hypothesis". Ann N Y Acad Sci 63: 15-43. PMID 13249313.
- ↑ Ritter RC et al. (1981). "Glucoreceptors controlling feeding and blood glucose: location in the hindbrain". Science 213: 451-2. PMID 6264602.
- ↑ Singer LK, Ritter S (1996). "Intraventricular glucose blocks feeding induced by 2-deoxy-D-glucose but not mercaptoacetate". Physiol Behav 59: 921-3. PMID 8778887.
- ↑ Warren JM et al. (2003). "Low glycemic index breakfasts and reduced food intake in preadolescent children.". Pediatrics 112: e414. PMID 14595085.
- ↑ Ball SD et al. (2003). "Prolongation of satiety after low versus moderately high glycemic index meals in obese adolescents.". Pediatrics 111: 488-94. PMID 12612226.
- ↑ Arumugam V et al. (2008). "A high-glycemic meal pattern elicited increased subjective appetite sensations in overweight and obese women.". Appetite 50: 215-22. DOI:10.1016/j.appet.2007.07.003. PMID 17714828. Research Blogging.
- ↑ Alfenas RC, Mattes RD (2005). "Influence of glycemic index/load on glycemic response, appetite, and food intake in healthy humans". Diabetes Care 28: 2123-9. PMID 16123477.
- ↑ Wynne K et al. (2005). "Appetite control". J Endocrinol 184: 291-318. DOI:10.1677/joe.1.05866. PMID 15684339. Research Blogging.
- ↑ Ahima R, Osei SY (2004). "Leptin and appetite control in lipodystrophy". J Clin Endocrinol Metab 89: 4254-7. DOI:10.1210/jc.2004-1232. PMID 15356017. Research Blogging.