Pseudomembranous enterocolitis: Difference between revisions
imported>Robert Badgett (Infobox with picture from c diff article) |
mNo edit summary |
||
| (44 intermediate revisions by 3 users not shown) | |||
| Line 1: | Line 1: | ||
{{subpages}} | |||
{{Infobox_Disease | | {{Infobox_Disease | | ||
Name = Pseudomembranous enterocolitis | | Name = Pseudomembranous enterocolitis | | ||
| Line 11: | Line 11: | ||
MedlinePlus = | | MedlinePlus = | | ||
}} | }} | ||
{{TOC|left}} | |||
In [[gastroenterology]], '''pseudomembranous enterocolitis''' is an "acute inflammation of the intestinal mucosa that is characterized by the presence of pseudomembranes or plaques in the small intestine (pseudomembranous enteritis) and the large intestine (pseudomembranous colitis). It is commonly associated with [[antibiotic]] therapy and [[clostridium difficile]] colonization."<ref>{{MeSH}}</ref> The disorder is an increasing matter of concern, as it is one of the more common [[nosocomial]] infections, but is also being seen in community-acquired cases. | |||
==Epidemiology== | |||
About 50% of patients with diarrhea after [[antibiotic]]s that is severe enough to be admitted to the hospital have pseudomembranes on [[colonoscopy]].<ref name="pmid17028914">{{cite journal |author=Lee KS, Shin WG, Jang MK, ''et al'' |title=Who are susceptible to pseudomembranous colitis among patients with presumed antibiotic-associated diarrhea? |journal=Dis. Colon Rectum |volume=49 |issue=10 |pages=1552–8 |year=2006 |month=October |pmid=17028914 |doi=10.1007/s10350-006-0694-z |url=http://dx.doi.org/10.1007/s10350-006-0694-z |issn=}}</ref> | |||
== | ==Diagnosis== | ||
[[Clinical practice guideline]]s address diagnosis.<ref name="pmid20307191">{{cite journal| author=Cohen SH, Gerding DN, Johnson S, Kelly CP, Loo VG, McDonald LC et al.| title=Clinical practice guidelines for Clostridium difficile infection in adults: 2010 update by the society for healthcare epidemiology of America (SHEA) and the infectious diseases society of America (IDSA). | journal=Infect Control Hosp Epidemiol | year= 2010 | volume= 31 | issue= 5 | pages= 431-55 | pmid=20307191 | |||
| url=http://www.ncbi.nlm.nih.gov/entrez/eutils/elink.fcgi?dbfrom=pubmed&tool=clinical.uthscsa.edu/cite&retmode=ref&cmd=prlinks&id=20307191 | doi=10.1086/651706 }} </ref> | |||
Sigmoidoscopy has a [[sensitivity and specificity|sensitivity]] of 31% in detecting pseudomembranes as compared to [[colonosopy]].<ref name="pmid7323683">Seppala, K, Hjelt, L, Supponen, P. Colonoscopy in the diagnosis of antibiotic-associated colitis. Scand J Gastroenterol 1981; 16:465. PMID 7323683</ref> | |||
[[ | |||
==Treatment== | |||
{{Seealso|Clostridium difficile}} | |||
==References== | ==References== | ||
<references/> | <references/>[[Category:Suggestion Bot Tag]] | ||
Latest revision as of 06:01, 8 October 2024
| Pseudomembranous enterocolitis | |
|---|---|
| Pseudomembranous enterocolitis | |
| MeSH | D004761 |
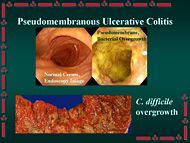
In gastroenterology, pseudomembranous enterocolitis is an "acute inflammation of the intestinal mucosa that is characterized by the presence of pseudomembranes or plaques in the small intestine (pseudomembranous enteritis) and the large intestine (pseudomembranous colitis). It is commonly associated with antibiotic therapy and clostridium difficile colonization."[1] The disorder is an increasing matter of concern, as it is one of the more common nosocomial infections, but is also being seen in community-acquired cases.
Epidemiology
About 50% of patients with diarrhea after antibiotics that is severe enough to be admitted to the hospital have pseudomembranes on colonoscopy.[2]
Diagnosis
Clinical practice guidelines address diagnosis.[3]
Sigmoidoscopy has a sensitivity of 31% in detecting pseudomembranes as compared to colonosopy.[4]
Treatment
- See also: Clostridium difficile
References
- ↑ Anonymous (2025), Pseudomembranous enterocolitis (English). Medical Subject Headings. U.S. National Library of Medicine.
- ↑ Lee KS, Shin WG, Jang MK, et al (October 2006). "Who are susceptible to pseudomembranous colitis among patients with presumed antibiotic-associated diarrhea?". Dis. Colon Rectum 49 (10): 1552–8. DOI:10.1007/s10350-006-0694-z. PMID 17028914. Research Blogging.
- ↑ Cohen SH, Gerding DN, Johnson S, Kelly CP, Loo VG, McDonald LC et al. (2010). "Clinical practice guidelines for Clostridium difficile infection in adults: 2010 update by the society for healthcare epidemiology of America (SHEA) and the infectious diseases society of America (IDSA).". Infect Control Hosp Epidemiol 31 (5): 431-55. DOI:10.1086/651706. PMID 20307191. Research Blogging.
- ↑ Seppala, K, Hjelt, L, Supponen, P. Colonoscopy in the diagnosis of antibiotic-associated colitis. Scand J Gastroenterol 1981; 16:465. PMID 7323683